AVM and Hiccup
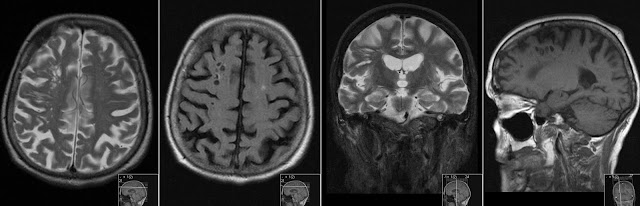
Patient presents with persistent hiccup since about a week. CT of the brain followed by CT Angiography (CTA) (not shown) revealed a large Arterio Venous Malformation (AVM) located dorsally to medulla oblongata and extending into the proximal spinal canal. Additional MRI investigation (above) has revealed a large thrombosed part of AVM that was not apparent on CT. Note two first images showing non-contrast T1 followed by two images after contrast. There is a large branch of the AVM stretching through the right foramen of Luschka (arrows) that shows high signal on non-contrast T1. The contrast enhanced T1 sequences show enhancement of the remaining parts of the AVM located posteriorly to medulla oblongata (arrowheads). High signal on non-enhanced T1 of the thrombus is due to free methemoglobin indicating about one week old thrombus. (Check my previous post about blood product signal on MRI). This corresponds with onset of patients symptoms - since the AVM was "silent" and already in place before.
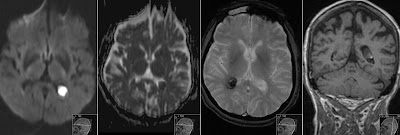
Also note on images above restricted diffusion from the thrombus seen on DWI. As usually first image is DWI (ep_b100t) then ADC (ep_b0_100) and T2 (ep_b0). Note high signal on DWI and low on ADC of this late subacute thrombus. Next stage in diagnostic imaging and therapy is conventional angiography.
Lesson from this case is that MRI is supplementary in diagnosis of intracranial AVMs and that it is very important to look at non-enhanced T1 since thromb can look just like patent AVM after contrast administration.
What concerns hiccups, let me quote an interesting article:
"Hiccup, nausea, and vomiting are thought to be caused by the lesions involving the dorsomedial medulla including the Area Postrema (AP) and Nucleus Tractus Solitarius (NTS), and the ventrolateral respiratory center (VRC) such as the nucleus ambiguus, although the neural network and its pathophysiologic relation to the symptoms in humans has not been fully understood." - Intractable hiccup and nausea with periaqueductal lesions in neuromyelitis optica - T. Mitsu
Neurology November 8, 2005 65:1479-1482